Self-funded workers’ compensation programs across the country are struggling to roundup the usual suspects that contribute to high program costs—namely medical and indemnity expenses, claims administration costs, litigation, and compliance with reporting requirements. Whether self-insured workers’ compensation programs perform these functions in-house or utilize a third-party service provider, they must control and oversee these processes in order to impact costs and outcomes.
Traditionally, self-funded workers’ compensation programs have been hampered by legacy systems that lacked contemporary automation capabilities and resulted in inefficient operations. These systems were highly resistant to change, interconnection with other systems and access by external third parties, such as claims specialists, loss-control experts, and attorneys.
Recognizing that today’s claims process must be flexible and extend beyond an organization’s four walls, program managers are beginning to leverage modern infrastructure to better support proven best practices. In fact, browser-based technology has become a means to automate operations, accelerate transactions, tightly manage quality and performance, and my business intelligence to continually improve program results.
Advanced Claims Automation
Since claims cost the property and casualty industry approximately $40 billion just to administer, it is a core insurance process that would significantly benefit from technological automation. In fact, it’s estimated that claim organizations spend as much as $11 – 14 billion in overpayment, waste, and inefficiency—or what the industry generally refers to as “claims leakage.” This leakage is primarily due to manual, paper-based operations and disparate information systems that result in less than optimal claims outcomes and poor customer service.
Browser-based claims technology helps organizations to achieve process transformation—moving from inefficient and disjointed operations to a more automated and integrated workflow. The following claims functions are now incorporated into a browser-based platform that exponentially increases the speed, efficiency, and cost-effectiveness with which claims are processed:
source: youtube
Online reporting of injuries. Prompt and accurate reporting of injuries is critical to achieving best-possible outcomes. With the Internet, injuries are now reported at anytime—24 hours a day, 7 days a week. Supervisors and managers who need to be notified of injuries can receive automated, immediate alerts on the same 24/7 basis. In addition, the development of “intelligent” online forms has made the reporting process easier. These smart forms use drop-down lists, auto-population of fields, and threads of logic to navigate users quickly through the electronic claims submission process. Due to its intuitive, user-friendly design, online reporting is often faster—not to mention less expensive—than a typical phone transaction.
A paperless paradigm. Today, the vision of paperless claims processing is finally being realized. In its rudimentary stage, self-funded programs may have scanned documents but continued to use paper to exchange information via fax and mail. To engage in a truly paperless paradigm, however, organizations are now avoiding the generation of paper documents, relying on electronic submission and exchange of information. In this data-driven environment, information is input once and made available to all parties via the browser-based infrastructure, which spans the entire enterprise and beyond, so third-party partners can also participate in a paperless claims process.
Consistent, quality claims handling. In the past, consistent claims handling was problematic; similar claims were often handled with widely divergent approaches and results. For example, with some complex injuries, the same case given to two different adjusters could produce a 100 percent variance in results. With business rules and workflow management, self-funded programs can consistently apply policies, procedures, and best practices throughout their organization to ensure quality results. Business rules also help to guide junior adjusters through an organization’s unique claims-handling process, essentially allowing them to receive training and handholding as they go.
Business rules enable straight-through processing. Ideally, claims organizations want to apply adjuster resources where they are needed most. By leveraging a sophisticated business rules engine, self-funded programs can increase their rate of straight-through processing. This means relatively simple and straightforward claims are settled with little or no human intervention. Claims adjusters are then free to focus their time and attention on more complex injury claims that require their expertise and personalized service.
The adjusters’ automation toolkit. Adjusters can utilize automation tools—such as automated forms, diary systems, scheduling tools, electronic communication, and prioritization of tasks—to help facilitate routine administrative functions, saving as much as 20 percent in adjuster time and resources. With these capabilities, adjusters can focus on tasks that directly impact costs and outcomes. For example, letter-writing and form-generation templates automatically produce documents with fields auto-populated from the claims database. Adjusters review, edit and send the documents, which saves time and automatically creates documentation within the claim.
Quality control through online audits. Claim departments have traditionally audited operations to ensure best practices are regularly performed. Since audits are time-consuming, they’re typically performed on a retrospective sampling of 10 – 20 percent of claims. With browser-based technology, online auditing enables greater transparency. Many organizations now perform real-time, concurrent reviews of 100 percent of their claims, enabling them to ensure a higher level of claims-handling performance. Audit findings then allow claim managers to fine-tune operations, achieve a tighter lifecycle and ensure cost-containment at key junctures of the claims process. Some entities have extended this function to also audit external service providers, such as medical providers and attorneys.
Technology to Manage Medical Costs
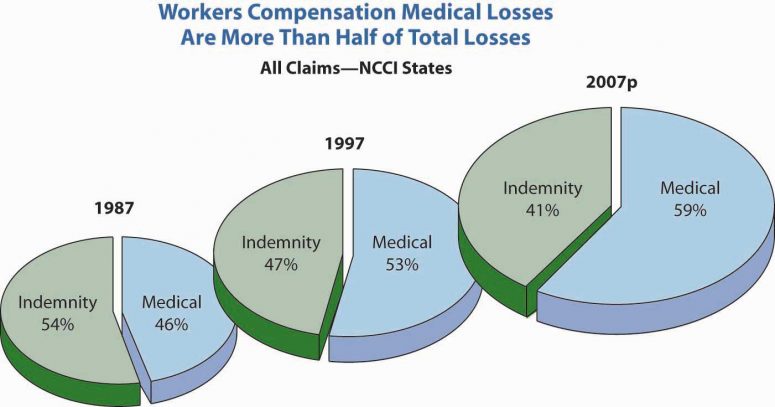
Double-digit medical inflation has affected workers’ compensation programs nationwide. In fact, medical expenses now account for approximately 60 percent of the costs of an average claim. To control these costs, self-funded programs are returning to tried-and-true medical management, but with a slightly new twist – leveraging a browser-based infrastructure to streamline and automate operations, as well as to provide the data analysis capabilities to improve outcomes:
Quality providers. The most critical component to effective medical management is utilizing an appropriate network of physicians who understand workers’ compensation requirements, return-to-work (RTW) objectives, and the importance of leveraging modified duty. Today’s latest data analysis tools can help organizations profile physicians to pinpoint providers who have the lowest overall claims costs and best outcomes. As employees are injured at work, technology helps direct these patients to quality providers in pre-established networks, ensuring the best delivery of care and the greatest level of provider discounts.

source: pinterest
Nurse case management. Nurse case managers should immediately be notified of urgent claims, so they can accompany injured employees to an initial medical visit; begin communication about RTW expectations and transitional work assignments; and help direct care to the extent allowed in the jurisdiction. Many of today’s nurse case managers are mobile or work from home. The latest browser-based technology allows them to access claims and medical information securely, at any time from anywhere—as well as to communicate and collaborate with claims management staff to enable optimal outcomes.
Medical bill review. Medical bills must be reviewed to ensure costs are billed in accordance with fee schedules, as well as provider discounts for additional savings. Bill review technology can update fees and discounts in real-time, ensuring the highest level of savings. In the past, medical bills and reports were housed separately from claims, creating silos of information that hampered efficiency. Today, medical bills and reports can be scanned and stored in one location and linked at the claims level to ensure the most complete claims and medical cost picture.
Litigation Management
Today, not only is the number of litigated cases growing, but average settlements are also rising. Generally, lawyer involvement drives up the cost of claims, but it does not increase the actual benefits paid to injured workers. As a result, it is in the interest of all parties to reduce litigation and lawyer involvement.
Rules to alert litigation specialists. The best defense to claims litigation is to enable highly qualified and experienced claims professionals to get involved early in a case to minimize the likelihood of litigation through up-front management. Business rules and alerts enable claims litigation specialists to ensure proper procedures are followed to evaluate claims and identify problems early on, so preventive measures can be taken.
Hyperlinks to share data with attorneys. When litigation must occur, communication and sharing of information with attorneys must be seamless. A browser-based platform provides hyperlink technology. A link can be sent via email, allowing attorneys to directly access claims information. These hyperlinks are secure and access rights are defined by the sender. For instance, a claims adjuster can email a hyperlink to the defense attorney. By clicking on the link, the attorney can connect to claim notes and can add information as well.
Analysis of litigation results. A browser-based platform also enables program managers to document and track judgments for plaintiff and defense counsels in order to identify trends and enable healthy competition among firms. For example, program managers may realize plaintiff counsel is targeting their employees, or certain defense firms may have a higher win rate.
Analysis for Safety & Injury Prevention
Safety and injury prevention is another critical component to optimizing workers’ compensation program performance. The key to success is identifying where losses are occurring and why, and to formulate a strategy to reduce and mitigate these incidents. To do this effectively, organizations require a 360-degree view of their risks and exposures.
In the past, there was no way to effectively collect and analyze loss information at an enterprise level; instead, risks were reported and monitored by the department. Many organizations utilized paper-based spreadsheets with data manually entered. These reports were time-consuming and labor-intensive to generate. They often relied on poor data, and since reports were not dynamic if information changed, someone had to update the corresponding files. In many cases, reports were delivered too late to effectively affect change.
Today, browser-based technology compiles all claims and loss information in one location and shares it with appropriate stakeholders. The resulting real-time business intelligence provides self-funded programs with the data to monitor claims activity and to recommend effective loss-control initiatives for high-cost and high-risk areas:
By regularly receiving and distributing reports, program managers systematically build awareness of program performance against defined goals and objectives. Business units and frontline managers can view departmental losses and compel respective divisions to follow policies and procedures to help reduce injuries. In this way, people at every level of an organization contribute to program success.
Supervisors use reports to identify departments with significant losses and work with these departments to reduce the frequency and severity of injuries. If a department has a high number of back-related claims, the department can respond with injury-prevention training or by providing safety equipment.
According to many industry experts, organizations that utilize advanced data analysis capabilities gain a greater awareness of risks and can save as much as three to 10 percent on their “total cost of risk” or TCOR – the costs to monitor the effectiveness of their risk management programs.
Continued Compliance with New Reporting Requirements
Finally, self-funded programs must ensure continued adherence with mandatory reporting requirements. Starting on January 1, 2011, many self-insured entities started to report claims involving Medicare beneficiaries to the Centers for Medicare and Medicaid Services (CMS).
Section 111 of the Medicare, Medicaid and SCHIP Extension Action of 2007 (MMSEA) has added these new reporting requirements, and meeting these requirements will be a huge undertaking. If claims are not reported appropriately, organizations may be fined $1,000 a day per claim. Self-funded entities must invest time, money and resources to understand the CMS guidelines, which are more than 200 pages in length. Many self-funded programs do not have prior experience with mandatory reporting procedures. Some lack the right data management and IT capabilities. Others do not want to rely on a reporting vendor to perform reporting on their behalf.
Whatever the situation, self-funded programs can utilize browser-based claims technology to self-report and thereby comply with MMSEA reporting requirements.
Rounding up the Usual Suspects
Workers’ compensation has been in a state of flux, but the usual suspects in terms of cost escalation remain the same. The critical new piece is utilizing technology to tightly manage and even improve program performance. Browser-based claims and risk management technology manages timely reporting of injuries, optimizes medical cost containment, and ensures best practices are consistently applied.
Program managers should realize that modern browser-based architecture has the ability to boost claims-handling efficiency and staff productivity. With a sophisticated IT infrastructure in place, self-funded program managers will be better equipped to put the usual suspects under lock and key. Many early adopters have already reaped the benefits: browser-based technology makes it easier for them to automate increasingly complex claims transactions, which involve multiple parties, multiple systems, and various regulatory requirements.
